While some people may need medication to manage their A1C (also called HbA1c), there are also many science-backed strategies that can help lower HbA1c levels naturally.

Please note: This article is not intended to provide medical advice, diagnosis, opinion, treatment or services. This article and the links contained in it provide general information for educational purposes only. The information provided in this article is not a substitute for medical care, and should not be used in place of the advice of your physician or registered dietitian.
TL;DR: How to Lower HbA1c Naturally
To lower HbA1c naturally, focus on small, sustainable lifestyle changes:
- Eat balanced meals with protein, fiber, and healthy fats to reduce blood sugar spikes.
- Walk for 10–15 minutes after meals and break up long sitting periods to improve insulin sensitivity. Add strength training twice per week to support muscle mass, your body’s natural “sponge” for glucose.
- Aim for a healthy weight and body composition by reducing body fat while preserving muscle.
- Get 7–9 hours of quality sleep on a consistent schedule with the same bedtime and wake-up time.
- Manage stress with simple daily practices like walking, breathing exercises, or journaling.
These habits often work synergistically: better sleep lowers stress, balanced meals fuel energy for movement, and regular activity helps keep blood sugar stable.
These approaches don't require drastic lifestyle overhauls. Whether you're dealing with prediabetes, type 2 diabetes, or simply want to optimize your metabolic health, these five practical steps could help you work toward more stable blood sugars, sustained energy, and better long-term health outcomes.
Jump to:
What is HbA1c?
Your HbA1c test reveals your average blood sugar levels over the past 2-3 months. Think of it like a school report card: a single test might show you did well that day, but the report card tells the truth about your overall performance. That’s HbA1c.
This blood test is used to diagnose pre-diabetes, type 1 diabetes, and type 2 diabetes. And if you already know you have diabetes, it is a good indicator of how much control you have of your diabetes.
A higher HbA1c means on average your blood sugar has been higher.
Save This Recipe! 💌
HbA1c Levels
In the US, an optimal A1c is 5.5% or less. The prediabetic range for A1c is 5.7% to 6.4%. The diabetic range is 6.5% or above.
In the UK or Ireland, if you have diabetes, an ideal HbA1c level is 48mmol/mol. If you're at risk of developing type 2 diabetes, your target HbA1c level should be below 42mmol/mol.
HBA1c Risks
It is important to keep your HbA1c at an acceptable level, as this will lower your chances of developing complications in the future.
Even individuals without diabetes may benefit from maintaining optimal HbA1c levels for better overall health and disease prevention.
The encouraging news is that you may be able to make meaningful improvements through practical, sustainable lifestyle changes that don't require perfection or extreme measures.
Step 1. Master the Art of Balanced Meals
One of the most common approaches people take when learning how to lower HbA1c naturally involves eliminating obvious sources of sugar. This includes removing sugar from coffee, avoiding desserts, and scrutinizing food labels.
While these steps can be helpful, they often miss the bigger picture.
Even foods typically considered healthy, such as oatmeal, fruit, or whole-grain bread, can trigger significant blood sugar responses. The key isn't necessarily avoiding these foods entirely, but rather learning strategies that may help minimize frequent spikes and crashes.
Focusing on blood sugar stability rather than eliminating carbohydrates can be an effective approach. This approach centers around creating balanced meals that combine protein, fiber, and healthy fats.
These nutrients work together as a natural buffer system, helping slow down how quickly your body absorbs sugar, potentially resulting in gentler, more sustained blood sugar responses.
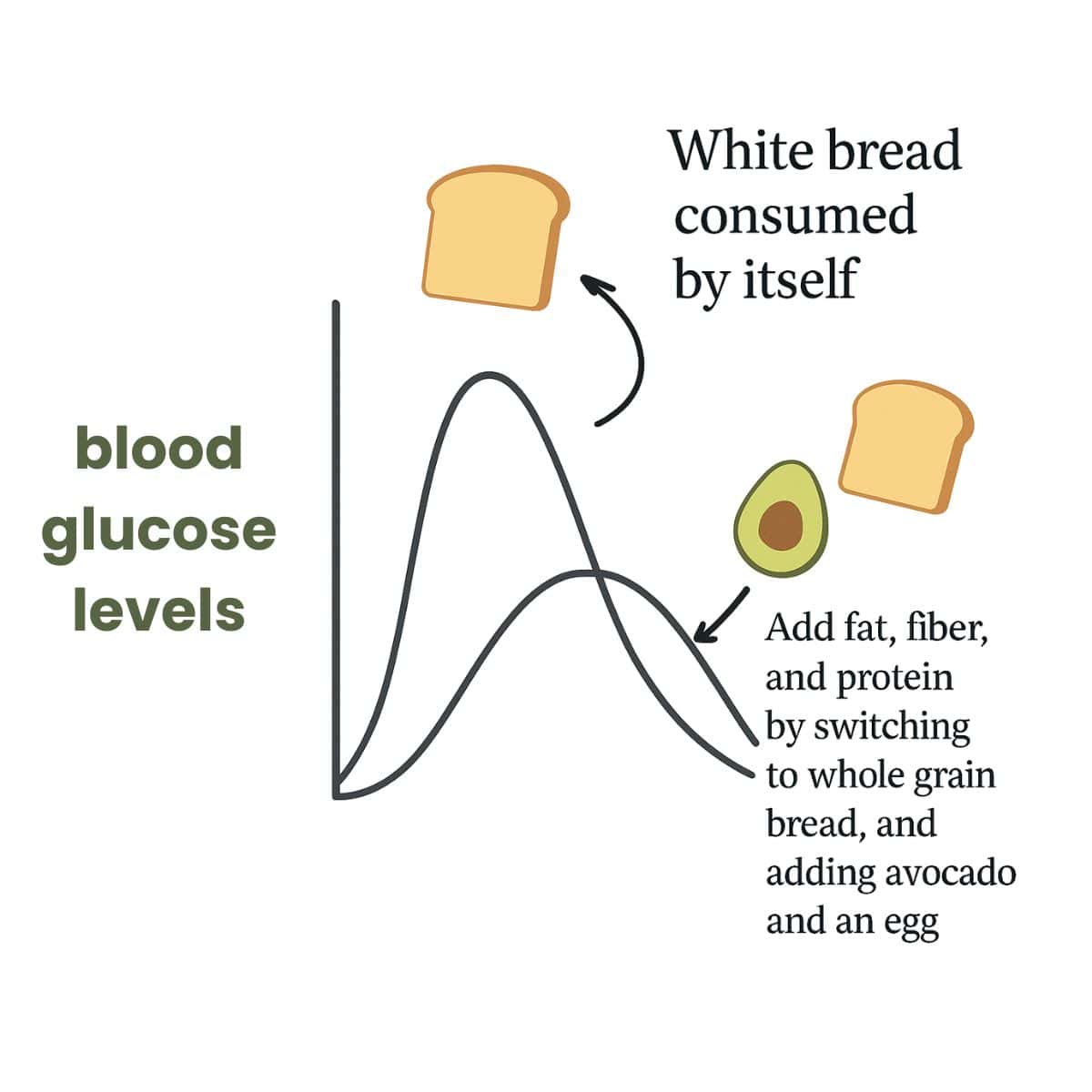
Over time, this steady approach could support healthier HbA1c levels without requiring extreme dietary restrictions.
Avoiding "Naked Carbs"
The above concept is sometimes referred to as avoiding "naked carbs". These are carbohydrates consumed without any accompanying protein, fiber, or healthy fats to moderate their absorption.
Here's how to apply this principle:
For fruit consumption:
- Pair bananas or berries with Greek yogurt, natural peanut butter or even my Greek yogurt fruit dip.
- Add nuts or seeds to fresh fruit servings
For bread and grain products:
- Top bread with avocado, eggs, cottage cheese, or nut butter
- Add protein-rich toppings like my high protein hummus, smashed chickpeas, or edamame
For snacks:
- Combine crackers with hummus or guacamole
- Choose protein-rich options alongside any carbohydrate-based snacks
This approach allows you to continue enjoying a variety of foods while potentially moderating their impact on your blood sugar levels.
Step 2. Optimize Your Movement Patterns
We all know how important regular physical activity is for our health. However when it comes to blood sugar management we can get even more strategic with how we approach this.
Research suggests that taking a 10-15 minute walk after meals may help reduce the blood sugar response from that meal. This happens because active muscles can utilize glucose for energy, potentially reducing the workload on your insulin system.
Over time, this could mean less glucose circulating in your bloodstream. Additionally, post-meal movement may aid digestion and help maintain steady energy levels throughout the day. Its a win-win!
To add to this we can try to avoid extended sitting periods as these may be detrimental to your health, particularly regarding blood sugar management. Many people remain seated at desks for hours without movement, which may allow blood sugar levels to gradually increase.
The solution is surprisingly simple: incorporate 2-3 minutes of movement every 30-45 minutes.
This could involve:
- Standing and stretching at your desk
- Walking to refill your water bottle
- Taking a brief walk around your office or home
- Simple desk exercises or leg shakes
Setting regular phone alarms can help establish this habit. Think of these as "exercise snacks" throughout your day. These small but consistent actions may help improve insulin sensitivity and support stable blood sugar levels.
Finally, we can aim to build muscle through resistance training.
After eating, up to 80% of blood glucose (sugar) is absorbed by your muscles, making muscle mass key for blood sugar management.
So while walking may provide immediate post-meal benefits, muscle tissue could offer continuous blood sugar support. Muscle functions like a glucose "sponge," potentially absorbing and storing sugar from your bloodstream.
Building muscle requires time and consistent effort, but the potential benefits extend far beyond blood sugar support. Increased muscle mass may support stronger bones, easier weight management, and improved overall metabolic health.
Step 3. Work Towards a Healthy Weight When Appropriate
Type 2 diabetes is strongly linked with carrying excess weight. One reason is that excess fat, especially around the belly area where we have the liver and pancreas can interfere with how these organs work, leading to higher blood sugars.
The good news is, even a modest 5–7% reduction in body weight combined with regular exercise has been shown in large studies to cut the risk of developing type 2 diabetes by up to 50%.
So there is huge possibility here.
However, the focus should be on reducing fat while preserving muscle mass, since muscle tissue may actively help with long-term blood sugar support, as mentioned above.
Weight Loss & Diabetes
When it comes to weight management in the context of prediabetes or diabetes, people often gravitate toward various eating methods: intermittent fasting, the carnivore diet, ketogenic diets, calorie counting, or low-carb approaches.
The reality is that multiple dietary strategies may facilitate weight loss when done safely and under proper guidance.
The critical factor is identifying an approach you can maintain long-term, because sustainability is what drives results. Consider these questions:
- What eating pattern fits realistically into my lifestyle?
- Which approach can I maintain indefinitely rather than as a short-term fix?
- What works best for my family situation and social commitments?
A1C & Low Carbohydrate Diets
Most of us eat more carbohydrates than our bodies really need, especially as daily activity levels have gone down. That doesn’t mean carbs are “bad,” but for some people, cutting back slightly can make a real difference for blood sugar and A1C levels.
What counts as “low carb” depends on who you ask, but many experts define it as anything under 130 grams per day (or less than about 26% of total calories). Typical intake often falls around 200–300 grams per day, so even bringing carbs down to 150 grams is considered a lower-carb approach. And the good news is that you can still enjoy foods like:
- Oats at breakfast
- Bread at lunch
- Potatoes at dinner
—all while seeing benefits. You don’t need to go as low as a ketogenic diet (around 20–50 grams per day) to get results.
The American Diabetes Association’s 2025 Standards of Care highlight this balanced approach. They:
- Recommend individualized eating patterns—no one-size-fits-all diet
- Recognize that lower-carb eating can help with diabetes management and prevention
- Encourage choosing nutrient-dense, high-fiber, minimally processed carbs instead of refined ones
Always work with healthcare professionals when making significant dietary or weight management changes.
Step 4. The Sleep-Blood Sugar Connection
Sleep quality plays a more significant role in blood sugar management than many people realize and can negatively impact HbA1c levels.
Research suggests that poor sleep habits could make blood sugars more difficult to manage, while elevated blood sugars may disrupt sleep quality. So its quite the viscious cycle!
The optimal sleep duration for adults ranges from 7-9 hours nightly. Both too little and too much sleep can be problematic for blood sugar management.
Improving Sleep Hygiene
Several simple strategies can go a long way toward improving sleep quality. I’ve actually written a full article on proven sleep tips, but here are a few of the biggest needle movers:
- Keep a consistent sleep schedule: Try to go to bed and wake up at the same time every day, even on weekends.
- Limit screen time before bed: Phones, tablets, and TVs can trick your brain into thinking it’s still daytime.
- Make your bedroom sleep-friendly: Keep it cool, dark, and quiet for the best rest.
- Wind down with a relaxing routine: Reading, stretching, or journaling can signal to your body that it’s time to sleep.
- Choose smart bedtime snacks: If you need a little something before bed, light snacks with protein and complex carbs may actually help.
However, if sleep problems persist despite these changes, consulting with your healthcare provider is important. Underlying issues may require specific treatment.
The Importance of Sleep Timing
Beyond sleep duration, timing matters significantly for blood sugar management too. Going to bed and waking at consistent times may support your circadian rhythm, which could help regulate insulin and cortisol levels more effectively.
Step 5. Stress Hormones and Blood Sugar
Stress management represents a crucial but often overlooked component when learning how to lower HbA1c naturally. When you experience stress, your body releases hormones like cortisol and adrenaline. This is part of our built-in survival system (picture a caveman sprinting away from a saber-toothed tiger).
This stress response may increase blood sugar to provide quick fuel for muscles. This worked well when stress meant fleeing from immediate physical threats.
However, modern stress tends to be chronic rather than acute. Work deadlines, financial pressures, family responsibilities, and constant digital notifications may keep cortisol levels elevated throughout the day.
When stress becomes constant but doesn't involve physical activity to utilize the released glucose, blood sugar levels may remain elevated. Over time, this chronic elevation could potentially drive HbA1c levels upward.
Additionally, elevated cortisol may influence where your body stores excess weight, potentially increasing the likelihood of abdominal fat accumulation. This is precisely where you don't want additional fat when managing blood sugar.
So trying to take a proactive approach to managing your stress can be hugely beneficial. I’m aware this is often easier said than done, but sometimes it just comes down to experimenting with what feels doable for you. This could be a short walk outdoors, five minutes of breathing exercises, or even learning to say no to something on your plate.
Conclusion
Learning how to lower HbA1c naturally doesn't require perfection or extreme measures. Instead, it’s about building small, sustainable habits that work together.
The best part? These strategies often reinforce one another. For example, better sleep can improve stress management, regular movement can support deeper sleep, and balanced meals can give you the steady energy you need to stay active. Over time, these connections create a positive cycle that supports both your blood sugar and your overall health.







Comments
No Comments